How To Become A Nurse
Nursing is a rapidly growing field with significant professional demand for qualified individuals. Even locally, there are many nursing schools in Philadelphia providing prospective career nurses to the surrounding established medical institutions.
This guide will provide helpful information on the steps to becoming a nurse, the educational and technical qualifications involved, and the position itself.
What Do Nurses Do?
Learn about the most common nursing duties, responsibilities, and procedures

Nursing is an honorable profession and an incredibly rewarding career path. Not only do nurses save lives, but they offer compassion and kindness to those that need it most.
They are often a source of comfort, safety, and security. If you are passionate about helping others, nursing may be a great career choice for you.
If you’re an aspiring Registered Nurse (RN) or Advanced Practice Registered Nurse (APRN), this article will cover some of the most common duties and procedures you may encounter throughout your career. We hope this information provides you greater inspiration while pondering a possible future in healthcare.
What Duties Do Registered Nurses (RNs) Have?
The Bureau of Labor Statistics (BLS) offers some insight into the most common roles and responsibilities of a Registered Nurse. Of course, these tasks can vary depending on your specialty, location, employer, and level of experience.
RNs typically perform the following duties:
- Assess their patient’s health conditions
- Record their patient’s medical histories and symptoms
- Monitor a patient’s health or recovery while recording their observations
- Administer medications and/or treatments to patients while under their care
- Develop or contribute to uniquely tailored patient-care plans
- Collaborate with physicians and other members of the healthcare team
- Operate and monitor medical equipment
- Perform and analyze the results of various diagnostic exams
- Teach patients and their families how to manage their illnesses or injuries
- Educate patients and their families on how to follow their prescribed treatment and recovery instructions upon returning home
Continue reading for a deeper dive into some of the specific duties and procedures typically performed by RNs and Advanced Nurse Practitioners.
1. Venipuncture
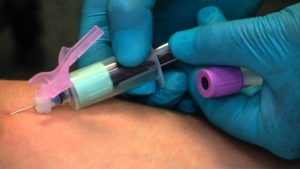
Some people refer to venipuncture as the most common invasive medical procedure. It’s essential for a number of medical diagnoses, procedures, and tests.
This important skill can be exciting for new healthcare professionals. It’s especially important for nurses to learn the proper methods for drawing blood, as well as the various methods and techniques for drawing blood in a healthcare environment.
What Is Venipuncture?
Venipuncture (or Phlebotomy) is the process of drawing blood intravenously from a patient. This is typically done by inserting a hollow needle into a patient’s vein to collect blood samples for laboratory testing.
In most scenarios, blood is drawn from a vein inside the patient’s forearm or the back of their hand. The procedure may be performed by nurses, medical laboratory scientists, medical practitioners, phlebotomists, dialysis technicians, and other nursing staff. Here are the steps they follow:
- Sterilize the site with an antiseptic wipe.
- Place an elastic band around the patient’s upper arm to apply pressure to the area (the vein will swell with blood).
- Insert a needle into the proper vein.
- Collect the blood in airtight vials or tubes attached to the needle.
- Remove the band from the patient’s arm.
- Take out the needle and cover the spot with a cotton swab/bandage to stop any bleeding.
When Do Nurses Perform Venipuncture?
Most nurses should learn venipuncture. While not always taught in nursing school, many programs recommend that aspiring nurses take supplemental courses to hone this skill.
Although most hospitals will rely on phlebotomy teams to perform this procedure, it is still vital for nurses to develop this skillset so that they may provide patients with the best care. In fact, nurses in some intensive care units are required to become proficient in venipuncture.
Generally, phlebotomy teams only make rounds at certain times in a hospital, so if there’s ever an urgent request for a blood sample, the responsibility for drawing that blood sample may fall in the hands of the hospital’s nursing staff.
2. Intubation
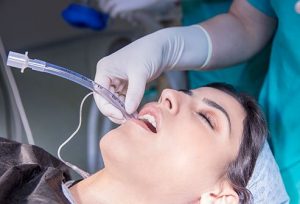
Intubation can mean the difference between life and death. This procedure is used to aid patients when they can’t breathe on their own.
Although intubation is not typically performed by most RNs, they are frequently administered by Nurse Anesthetists and other Advance Practice Registered Nurses (APRNs).
What Is Intubation?
When it comes to airway management, learning how to intubate is key. Endotracheal intubation is the process of inserting a tube through the patient’s mouth and into their airway. This is done for patients who need to be placed on a ventilator during anesthesia, sedation, or severe illness.
When Do Nurses Perform Intubation?
The frequency by which nurses perform intubation greatly depends on their location. A nurse’s scope of practice is defined by their state’s nursing rulebook, more technically referred to as the state’s nursing practice acts.
For Advanced Practice Registered Nurses, such as Nurse Practitioners or Nurse Anesthetists, intubation is commonly included in their scope of practice. For Nurse Anesthetists, for example, intubation is the primary means through which they deliver anesthesia in the operating or delivery room.
However, some states, like Nevada, may allow RNs to intubate if they have completed special training (i.e. advanced cardiac life support training). In addition, nurses who work in emergency medicine or air-and-surface transport may also be allowed to intubate patients.
3. Blood Transfusion
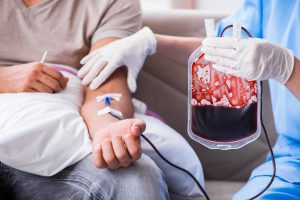
Blood transfusion is a potentially life-saving procedure that replaces blood lost during surgery or injury. A blood transfusion can also serve as a treatment for patients with illnesses that stifle their ability to naturally produce enough blood cells for their bodies.
What Is a Blood Transfusion?
Blood transfusions are a routine medical procedure that delivers blood into a patient’s body through a narrow tube that’s connected to a vein in their arm or hand.
To administer a blood transfusion, healthcare professionals place a thin needle into a vein—usually located in the arm or hand—which allows blood to move from a bag, through a rubber tube, and into the patient’s vein through the needle. Nurses must closely monitor their patient’s vital signs throughout this procedure.
When Do Nurses Perform Blood Transfusions?
Nurses often perform blood transfusions under the direction of a doctor’s order. Nurses Labs outlines this process in detail, but here are the first seven steps that nurses typically follow:
- Verify the doctor’s order. Inform the patient and explain the purpose of the procedure.
- Check for cross matching and blood type to ensure compatibility.
- Measure the patient’s vital signs.
- Practice strict asepsis.
- At least two RNs should check the label of the blood transfusion to review the following information:
- Serial number
- Blood component
- Blood type
- Rh factor
- Expiration date
- Screening test (VDRL, HBsAg, malarial smear) – This is to ensure that the blood is free from blood-carried diseases and, therefore, safe for transfusion.
- Blood for the transfusion should be warmed to room temperature to prevent chills.
- Prepare a needle for the transfusion using a needle gauge of 18 to 19 to allow easy flow of blood.
Where Do Nurses Work?

Not all registered nurses work in hospitals. You can find a nurse in a wide variety of health care settings, including doctor’s offices, urgent care centers, pharmacies, schools, and many other locations.
Nurses have the ability to use their skills to meet the needs of their patients, pretty much wherever they are located. For example, many nurses now assist the elderly or disabled in their homes. Some common places where nurses work include:
- Hospitals
- Clinics
- Offices
- Schools
- Pharmacies
- Ambulance/Helicopter
- Home health care settings
- Senior living communities
Types of Nurses (with Requirements)

Answering the question of what do nurses do can be challenging due to the fact that nurses are skilled in many fields and may choose to focus their trade specifically in certain types of care. Some specific nursing fields include geriatrics, critical care, pediatrics, treatment planning, and case management.
From working face-to-face with patients to managing their paperwork, nurses play a huge role in our lives and the profession continues to be a prosperous career path for those considering taking on this role. Some different types of nurses and their education requirements include:
- Nurse Anesthetist. A nurse anesthetist assist mainly with medical procedures, specifically with anesthetic. To become a nurse anesthetist, you must hold bachelor’s degree.
- Family Nurse Practitioner. A family nurse practitioner delivers family-focused care as a part of a healthcare team. Family nurse practitioners must hold a master’s degree.
- NICU Nurse. A NICU nurse works with sick newborn babies. To become a NICU nurse, you must hold a bachelor’s degree.
- Labor and Delivery Nurse. A labor and delivery nurse assists with the birth of newborns. Labor and delivery nurses must hold an associates degree.
- Travel Nurse. A travel nurse works short-term contracts in multiple locations in order to explore the world while working as a nurse. To become a travel nurse, you must hold an associates degree.
- Neonatal Nurse. A neonatal nurse works with sick babies. Neonatal nurses must hold a bachelor’s degree.
- Pediatric Nurse. A pediatric nurse works with children in maintaining their normal care. To become a pediatric nurse, you must hold an associates degree.
- Ambulatory Nurse. An ambulator nurse works specifically on an ambulance for numerous emergencies. Ambulatory nurses must hold an associates degree.
- Clinical Nurse Specialist. A clinical nurse specialist works with patients in a variety of specialties in an advanced setting. To become a clinical nurse specialist, you must hold a master’s degree.
- School Nurse. A school nurse provides medical support, education and treatment within an adolescent school facility. School nurses must hold an bachelor’s degree.
- Nurse Educator. A nurse educator instructs and teacher aspiring nurse and health professions in their journey towards their career. To become a nurse educator, you must hold a master’s degree.
Becoming A Nurse in Nigeria: there are several areas where nurses specialise in Nigeria, namely
- Accident and Emergency Nursing
- Anaesthetic Nursing
- Orthopaedic Nursing
- Mental Health Nursing
- Obstetrics and Gynaecological Nursing (midwifery)
- Ophthalmic Nursing
- Cardiothoracic Nursing
- Renal Nursing
- Peri-operative Nursing
- Critical Care Nursing
- Occupational Health Nursing
- Clinical Research Nursing
- Pediatric Nursing
- Geriatric Nursing
- Public Health Nursing.
Nurses who have already undergone General Nursing training and have been certified to practice in Nigeria can enroll for these training in schools of post-basic nursing.
Most of these programs run for a period of one year, while others run over 18 months to 2 years.
There are interesting employment’s opportunities for nurses in Nigeria.
HOW TO GET A JOB AS A NURSE

Hardly Does A Nurse In Nigeria Go Without A Job For More Than A Month
However, the career prospects and remuneration is largely dependent on the specialty, years of experience, skills and clinical competence, and in some cases level of education.
Job opportunities are available in the intensive care unit, for critical care nursing specialist, which may be for an adult, or a pediatric Intensive care unit (ICU).
Pediatric nurses can also work in the pediatric ICU if they have some years of experience and competence in the pediatric specialty.
General nurses have employment opportunities in general medical and surgical units.
Perioperative nurses work in the theatres alongside surgeons.
Anesthetic nurses also work in critical care units as well as in the theatre, administering anesthesia, and nursing the patient to recovery in the post anesthetic care unit.
Midwives can work in labour wards, maternity homes, or in the community, along with public health nurses at primary health care levels.
Renal nurses work in dialysis units, and kidney transplant center’s, caring for patients with kidney diseases undergoing dialysis, or kidney transplant, or other invasive procedures involving the kidneys, such as kidney biopsy.
Occupational health nurses in Nigeria work in industrial sites and factory clinics, to provide first aid treatment for work-related hazards and injuries sustained at work.
HOW MUCH ARE NURSES PAID?

Apart from the opportunities in clinical practice available to nurses in Nigeria, there are job roles nurses take up outside their conventional clinical duties
Health insurance is one amazing route nurses ply in Nigeria, pursuing their career.
They work in different units in private health insurance companies, commonly in the call centre, where they interface between the company, patients and hospitals that provide patients’ care.
Clinical research is also another viable career pathway that is available to nurses in Nigeria, although there are limited opportunities in this area.
Nurses can secure positions as clinical research nurses, coordinating the processes of clinical research, alongside a principal investigator.
Such opportunities are available in research institutes in Nigeria, such as the Nigerian Institute of Medical Research, as well as some international research organizations with sites in Nigeria.
Finally, nurses can also work as educators and university professors in schools and colleges of nursing across Nigeria.
Nurses in Nigeria only earn modest incomes, a few that have very good employers, or work in very lucrative specialities earn handsomely, while those who work in privately owned healthcare facilities in rural areas earn below the margin.
On average, nurses that work in the public health sector earn more than those in the private setting.
A new starter, with a general nursing certificate, earns an average of N70,000 (approximately 184 U.S. dollars), a pediatric nurse, like most other specialist nurses, earns an average of N100,000, while critical care nurses, as well as anesthetic nurses, earn an average of N140,000.
A clinical research nurse earns an average of N110,000.
Nurses that work in health insurance companies earn an average of N120,000.
The income is not a fixed price in private parastatals, as there is no fixed scale.
Every management determines what to pay its employees.
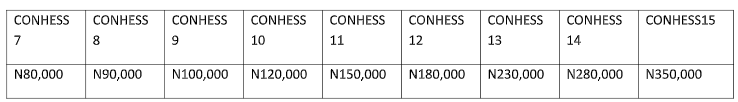
However, for the public health sector nurses in Nigeria, the income is relatively stable as they are paid on a standard salary scale called CONHESS (Consolidated Health Salary Structure).
The pay scale for nurses in Nigeria according to National salaries income and wages commission (2009) is summarized in the table below
HOW TO ADVANCE MY CAREER AS A NURSE.
Here are some experts’ top tips for advancing your own nursing career:
1. Invest in your education.
“Education is extremely important in advancing one’s career. With each degree in nursing or certificate in a specialized nursing program one has more options for new opportunities. With more opportunities, it is more likely that one will find a position that is a perfect fit,” offered Schepp.
She also encourages nurses who need to simultaneously work and go to school to take advantage of the stepladder approach to nursing education, which can allow working as a LPN while pursuing an associate’s degree in nursing, and then to work as a RN while completing a bachelor’s degree.
Ambler and Weber both emphasized the increasing importance of advanced degrees, citing that most positions in advanced practice, leadership, teaching and research require master’s and doctoral degrees.
Additionally, Ambler suggested that nurses looking to advance in management focus more on obtaining certifications pertaining to management, such as those offered by the American Organization of Nurse Executives (AONE) and the American College of Healthcare Executives, rather than clinical certifications.
Fuller added that the University of Phoenix offers unique dual degrees: a MSN/MBA which provides the master’s level nurse with a background in business fundamentals and a MSN/MHA which provides a background in health administration.
“A more educated nurse is a safer nurse. Education requires a commitment. It is a personal journey that takes time and energy, but it also provides rewards, both professionally and personally,” she reflected.
2. Build and utilize your networks.
“Learn to network within your health care organization and outside it. By meeting new people, you exchange ideas and gain information about new approaches to solve common problems. Take something you care about as a nurse and focus on networking with others who share this same interest,” advised Weber.
Fuller recommends taking opportunities to join professional networks such as Sigma Theta Tau International Honor Society, the American Nurses Association and your state’s nursing association.
“Professional social networking is also becoming increasingly crucial in our society,” said Fuller. “As the world has changed, global networking and community networking is becoming more central to how we do business. It’s the wave of how people are connecting across disciplines.”
While networking is clearly important for career advancement, it should also be seen as a source of learning and new ideas.
“A network of colleagues can be supportive and informative,” stated Schepp. “One can build a network by attending conferences or workshops with others who have similar interests, reading journal articles and blogging with each other, holding reading groups, or participating in webinars with colleagues.”
3. Establish a mentoring relationship.
“It takes time to develop a mentor-mentee relationship and it cannot be forced. However, a nurse can take some steps to become a mentee by first identifying someone whom they feel comfortable with and whom they consider a role model,” advised Weber. “Asking the mentor for career advice, suggestions and guidance is a good way to initiate the relationship.”
Ambler expressed that he would be impressed if a nurse asked for mentoring—so don’t be afraid to state interest in receiving wisdom, advice and coaching from a successful professional.
“I’m in the school of thought that you shouldn’t be mentored by someone with whom you work directly, especially not the person you report to,” he remarked. “I see great value in seeking a mentor outside of health care because they can offer fresh perspectives on managing people and resources.”
There are some formal mentoring programs run by organizations such as AONE, but there are a number of ways to seek out mentorship like asking a professional you admire for assistance on a project or for words of wisdom. Schepp also suggests joining research groups, journal clubs and volunteering on special projects as avenues to meet people who can mentor you.
4. Always pursue professionalism.
Schepp lists the key components of nursing professionalism as being honest, maintaining confidentiality about patients, offering respect for the individual, cultivating strong interpersonal skills in dealing with people, keeping a positive attitude, maintaining competency and keeping up to date in one’s work.
Fuller sees ethics as the cornerstone to nurse professionalism, “Nurses at every level and every position need to understand ethics and the role of ethics in their practice. As nurses, we influence the decisions and health of our patients. Ethics needs to be at the forefront of those decisions.”
It is important for nurses to present themselves as professionals both on the job and off.
“It is common practice for employers to look at a candidate’s Facebook page or personal website. The pictures and content in these pages give another perspective of the candidate than the one obtained from an interview,” explained Weber. “Having been on numerous search committees, I have seen first-hand a candidate removed from consideration after a committee member viewed their personal website.”
5. Continue personal and professional development
Developing yourself as a person will also have a positive impact on your career. Schepp recommends focusing on communication skills such as conflict management, active listening and clear, effective writing, as well as honing skills in problem solving.
“I urge nurses to see themselves as leaders and to personally cultivate and promote their leadership skills and abilities,” Weber said. “Begin cultivating your leadership within your own health care setting. As you become comfortable as a leader, look for other opportunities both within and outside your organization.”
Further words of wisdom
“Some over-arching advice I would offer is to find what you like to do in your career and do the best job possible and seek out work environments that are positive and growth promoting,” Schepp concluded.
“Keep your eye out for nursing positions that fall outside what you are doing now,” Weber added. “Job advertisements and articles about nurses in other settings will open your thinking about career opportunities. Since 50 percent of nursing positions are outside the hospital, and since health care reform will result in new and as yet unknown job opportunities for nurses, expanding your perspective may lead to an exciting job possibility in the near future.”